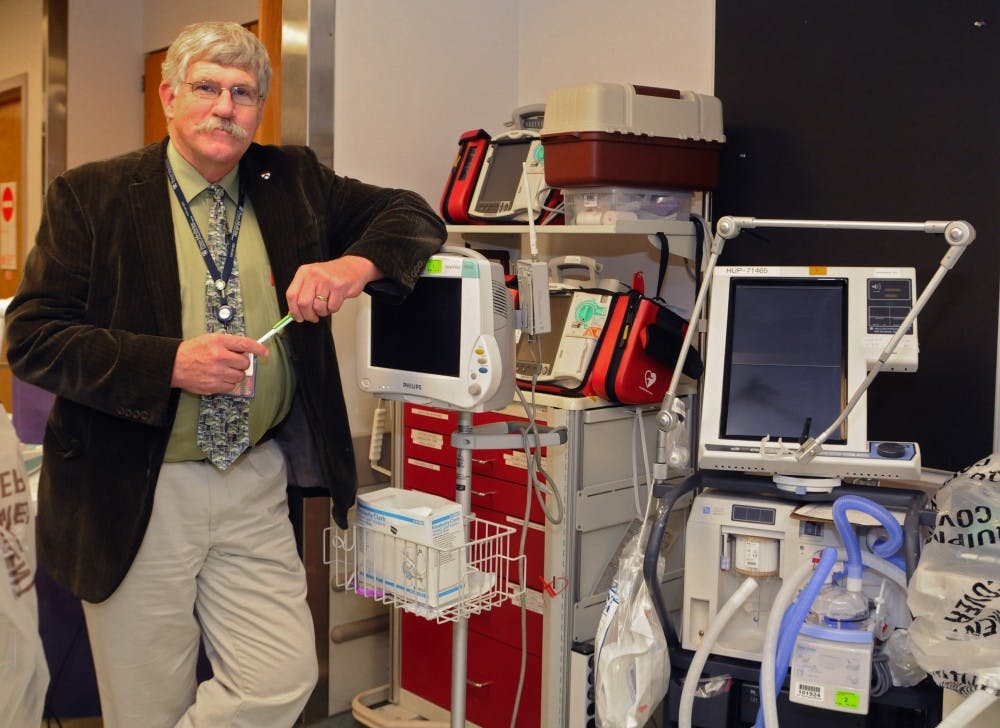
In 14 hours, Jim Browning broke up a family fight, worked on a homicide investigation, slept no more than three hours and walked, by his approximation, several miles.
Browning, coordinator of Clinical Pastoral Education at the Hospital of the University of Pennsylvania, was working his monthly night shift as the only on-call chaplain in the hospital.
His duties include anything from leading family prayers and consulting on treatment decisions to serving as the official liaison between doctors and the families of trauma patients.
He’s wearing a blazer and tie — the usual uniform for an on-call night. He also carries a pager, and walking with him, one would think the whole world has his number. When a trauma is reported, he receives a page and the patient’s estimated time of arrival.
On that night, I left his office around midnight, but Browning promised to call me if there was a trauma later. He wanted to get some rest because his evening had been very difficult. Earlier that night, a family fight erupted after a mother of 11 died. “We all do funny things with our grief,” he said.
At 1:56 a.m., I got a call that a trauma patient from a motorcycle accident was on his way to HUP. He asked, “Could you be down in seven minutes?”
***
Pastoral care at HUP is hardly a modern innovation. The hospital has embraced some kind of religious presence since the late 19th century, when the Board of Women Visitors first hired local clergy members to visit patients. Since then, the Department of Pastoral Care has made a permanent mark on the hospital’s culture, emphasizing interfaith religious care and “spiritual research” — programs that find connections between a patient’s spirituality and healing.
Director of Pastoral Care Ralph Ciampa said having on-call chaplains at the hospital can be crucial to a patient’s healing, especially when “it’s tough for [local ministers] to follow the exact status of a patient.”
No matter their spiritual bent, however, trauma patients value very much when someone prays for them, at times when they are at the “ragged edge of panic,” Ciampa said.
“We’re happy providing care whether it looks religious or not,” he added.
I arrived at HUP shortly after 2 a.m. Browning met me in the emergency waiting room and led me down into the trauma bay — a small wing off to one side of the Department of Emergency Medicine where trauma patients are received and given immediate intensive care.
A “trauma,” Browning said, is what he calls a patient in a very serious condition. Browning had already seen two other traumas that night: a man hit by a car, and younger woman who had fallen off her bike and fractured her skull.
The motorcycle trauma had arrived before I stepped into the trauma bay. Doctors had removed the patient’s clothes and laid him on a gurney. Earlier that night, Browning had described to me the movements he must make to weave his tall frame through doctors in the trauma bay.
“It’s really like a ballet,” he said. “Each dancer has a spot.”
Browning’s mission is to gather as much personal information about the patient as he can and notify the family. If the patient is incoherent or unconscious, he will either look in the patient’s clothes for a cellphone, or speak with witnesses and paramedics.
A hospital chaplain can’t relay medical information to patients’ families. He can only tell them that there had been an accident and that a family member is in the hospital.
While we were by the phone, another patient was rushed into the bay. The patient had suffered several gunshot wounds. Again, Browning shuffled to the patient’s gurney, asking for a name or any useful information.
After several minutes Browning returned to where I stood, near the entrance of the trauma bay, and leaning close to me, said, “That patient is dead.”
***
Around 2:30 a.m. the gunshot victim’s family arrived.
When Browning or another chaplain accompanies a nurse or doctor in the family waiting room, he must prepare himself and his appearance to make things run “a little smoother,” he said.
“Smoother,” however, sometimes needs some creativity. For instance, Browning flips his name badge, which very clearly labels him a chaplain, so as not to alarm the family when he comes into the waiting room.
“Sometimes when a family sees that’s what I am, they look at me and think, ‘Dead,’” Browning said.
However, he believes his main role in the waiting room is to be “a third ear,” who can clarify for family members what the doctor said and even, if need be, catch a fainting mother.
Through all the tears and grief, Browning keeps up morale with lighthearted humor and an uncle-like demeanor.
“We try to make sure no one goes through this alone,” he said. “We work alongside the doctors for the best of the family. And the docs trust us.”
As coordinator of the CPE, Browning is also a teacher. He has 18 students, ranging from 29 to 68 years old, who work in various units of the hospital to earn their chaplaincy accreditation. Each student also takes the 14-hour night shift three or four times per month. Browning, who had been the first full-time Director of Pastoral Care at St. Jude Children’s Research Hospital in Memphis, Tenn., and director of CPE at a senior care facility in the Harrisburg area, has only taught at HUP for a year and a half, but desires to show “good modeling” for his students.
He still takes monthly shifts to maintain his skills and also to relate to his students undergoing training.
Each night, the on-call chaplain keeps a log detailing the night’s events. When Browning presents his log the morning after a shift — a procedure called “processing” — his students offer both emotional support and constructive feedback.
Browning believes the CPE program, and his role as a teacher, hinges on his students’ ability to learn from their mistakes and constantly adapt their vantage points in difficult situations.
***
At 3:25 a.m., Browning received another page. A nurse had asked him to deliver the motorcycle trauma patient’s wedding ring to his mother. The patient was awaiting surgery on another floor.
Browning met the nurse by the elevator then walked down to the waiting room to meet the mother.
After giving her the ring, the three of us searched the hospital for another waiting room where the mother could rest and watch TV. Browning had another five hours to go before regrouping with his students. Walking into an elevator, he made some gentle small talk with the mother, to calm her nerves.
“Not the best thing to wake up to, is it?” he said. The mother, visibly exhausted, laughed.
Related
Nursing School Task Force maintains presence in Haiti
Penn for Jesus constructs prayer tent on College Green
Reporter’s Notebook | An evening with MERT
The Daily Pennsylvanian is an independent, student-run newspaper. Please consider making a donation to support the coverage that shapes the University. Your generosity ensures a future of strong journalism at Penn.
DonatePlease note All comments are eligible for publication in The Daily Pennsylvanian.





