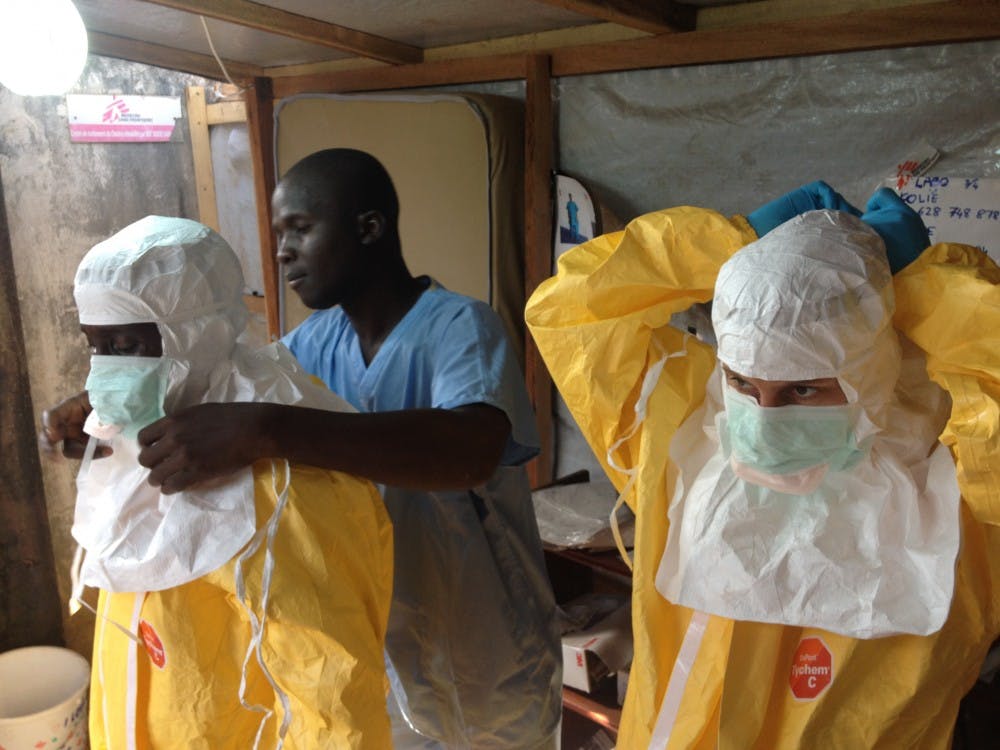
"Ebola in Ghana" by European Commission DG ECHO is licensed under CC BY 2.0
As the Ebola outbreak continues to devastate Western Africa, Penn students and researchers tackle the challenges of helping prevent the spread and dangers of the deadly virus.
One organization called Power Up Gambia confronted Ebola hands-on this summer by helping local hospitals and clinics in The Gambia, a West African country, secure energy sources by donating and installing solar panels.
Because of PUG’s partnership with The Gambia’s Sulayman Junkung General Hospital, Power Up Gambia continually sends students to the region to assist Gambian hospital staff and patients.
However, according to Executive Director of Power Up Gambia Lynn McConville , the increasing death toll and severity of the Ebola outbreak puts Penn students in the region in serious danger.
The Center for Disease Control describes the outbreak as one of the largest in the history of the Ebola virus, estimating over 3,000 cases and 1,500 deaths as of Aug. 28. The Gambia lies fewer than 100 miles from Guinea, one of the sources of the Ebola outbreak.
Countries nearby the Ebola outbreak are dealing with supply shortages and lack of proper equipment to prevent the Ebolavirus from traveling across borders, McConville said, with basic items like gloves and face masks low on stock.
Although health checks are being implemented at country borders to prevent people in nearby countries like The Gambia from catching the virus, the regular thermometers used to prevent the spread of the virus are not as successful as infared thermometers.
But, with supply shortages, using infared thermometers is not a feasible option.
“Millions of dollars are going towards the outbreak but not towards surrounding countries like The Gambia,” McConville said. She hopes that solar suitcases, which provide portable energy, can be used to power the infrared thermometers in the near future.
But it’s possible that some of the fears over the spread of Ebola are unfounded, according to Darren Linkin , assistant professor of medicine in the Division of Infectious Diseases at the Perelman School of Medicine.
Ebola spreads through contact with blood and other infected bodily fluids, and its symptoms are similar to those of fevers caused by other etiologies, putting Ebola on a long list of potential diagnoses.
“What if there were a patient who said, ‘I have fever, headache, non-specific symptoms and I was just in Nigeria for business?’” he said. These symptoms could also be due to malaria or the flu, he explained, revealing the need to rule out alternatives before jumping to Ebola.
However, the fear of Ebola spreading throughout West Africa is a larger concern than fearing it will spread to the United States, according to Chair of the Department of Medical Ethics & Health Policy and Vice Provost for Global Initiatives Ezekiel Emanuel .
American health facilities have proper infrastructure to control infectious diseases, but the affected African countries do not have similar advantages, he said.
“We have health systems that are overwhelmed, dealt with civil war and inability to train,” Emanuel said.
Linkin said that an outbreak in America is enough of a possibility to take precautions. As the hospital epidemiologist at the Veteran’s Administration Medical Center, he has helped ensure that Penn medical facilities are capable of treating patients infected by the Ebolavirus.
As an extra measure, Linkin provides guidance to emergency department personnel who would need to be the first to identify a patient infected with Ebolavirus.
However, Linkin believes that there’s little reason to worry about an American outbreak. The CDC also maintains that the threat of an Ebola outbreak in America is not significant.
“People don’t worry about the mundane things that are causing more illnesses,” Linkin said.
Penn is also on the forefront of new research to treat Ebola and other highly contagious and deadly illnesses, which could help reduce the fears of Ebola spreading.
In a lab within Penn Vet, Associate Professor of Microbiology Ronald N. Harty has been studying Ebolavirus models since 1998. Harty works with the matrix proteins of the virus, which assemble into particles that can bud off from the original host cell and infect other body cells. His lab focuses on finding compounds that could block the budding process.
“A virus hijacks host proteins and uses it for its own purpose to facilitate the budding process,” Harty explained. “We can block the interaction with a small compound or antiviral drug and have the viral particle dangling outside of the cell, but cannot quite break free.”
A dangling viral particle would be recognized by the host’s immune system, and so Harty’s compounds essentially buy time for the host to mount a counterattack.
The translation of Harty’s findings into a drug against Ebola is still far from reality. Harty must first prove that the treatment works on animals, and then make it safe to use on humans.
The way Ebola spreads throughout the body is similar to how rabies and HIV spread. “The exciting part there is that a drug that can block Ebola can also block HIV,” Harty remarked.
The Daily Pennsylvanian is an independent, student-run newspaper. Please consider making a donation to support the coverage that shapes the University. Your generosity ensures a future of strong journalism at Penn.
DonatePlease note All comments are eligible for publication in The Daily Pennsylvanian.





